Digital Healthcare Payer Platform to Better Understand ICP (Ideal Customer Profile)
September 6, 2023 | 2-minute read

Our recent webinar, hosted by Health Chain CEO, Sudheen Kumar, and the VP of Strategy, Mason Burr, provided perspective into the possibilities that are now more attainable than ever for health plans in understanding their Ideal Customer Profiles.
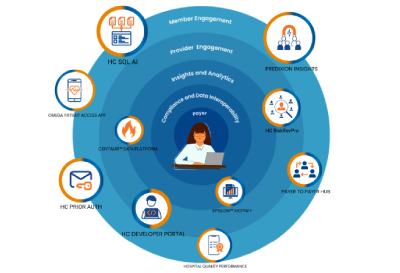
Sudheen Kumar shared his vision for the Health Chain Suite: "Our goal is simple yet profound – to empower Health Plans with tools that provide an unparalleled understanding of their membership. The Digital Healthcare Payer Platform we've built serves as a gateway into the heart of every Health Plan's Ideal Customer Profile."
The crux of this platform lies in its exceptional use of advanced data analytics and machine learning. By tapping into historical leads and sales data, Health Plans can unearth valuable member acquisition and conversion trends. Mason Burr, the VP of Strategy, called the Predixion Insights AI-driven tool ‘a game-changer’– our insights empower Health Plans to tailor and prioritize member acquisition campaigns with laser-like precision. It's all about quality engagement over quantity."
A pivotal aspect of Predixion Insights is its capability to identify the perfect prospects for the right health insurance products based on population-level trends. The power of prediction is invaluable in deciphering the needs of the future and the Predixion platform isn't just about insights; it's about foresight.
But what truly sets Predixion Insights apart is its’ predictive prowess. The platform analyzes patterns in engagement + interventions to identify member engagement preferences, care plan tendencies and potential gaps in care that require intervention to ultimately optimize member engagement, reduce churn and increase Star Ratings. Picture having an integrated view of members, categorized seamlessly by risk of disenrollment, urgency, you name it. As healthcare navigates through the currents of change, Predixion Insights is the compass directing the member experience.